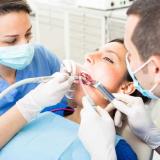
If your child is past age 5 and still wetting the bed, you are probably exhausted. You have tried limiting water before bed, setting alarms, and staying positive. But the accidents keep happening.
Here is something most parents are never told: the most effective bedwetting treatment may have nothing to do with the bladder at all. It may start with the way your child breathes during sleep.
At Chester Dental Care , we work with families in Chester, VA, and the surrounding Richmond area who are finding answers by looking at the connection between bedwetting and sleep-disordered breathing (SDB). Once the breathing is addressed, the bedwetting often stops on its own.
Disclaimer: This article provides general information and discussion about health and related subjects. The information provided by Chester Dental Care is not medical advice and is not intended to be a substitute for professional medical advice, diagnosis, or treatment from a qualified medical provider, physician, or specialist. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.

Key Takeaways
-
Reasons for bedwetting go beyond development. If your child is still wetting the bed after age 5, sleep-disordered breathing may be a contributing factor, not just a slow developmental timeline.
-
Bedwetting and sleep apnea are closely linked. Research shows up to 80% of children with nocturnal enuresis also have obstructive sleep apnea (OSA).
-
When breathing is interrupted during sleep, the brain loses some control over bladder function, which is one of the key reasons bedwetting persists despite other interventions.
-
Bedwetting treatment that targets the airway, not just the bladder, often produces better results. Addressing the root cause of disrupted breathing is where lasting improvement tends to come from.
-
If you've been asking how to stop bedwetting and nothing has worked, look for signs like snoring, mouth breathing, or restless sleep. These are worth raising with a dental or medical provider who understands airway health.
What Is Bedwetting, and When Should Parents Take Notice?
Bedwetting, also called nocturnal enuresis, is when a child urinates during sleep without waking up. It is common in toddlers, but it should taper off as a child gets older.
Bedwetting that continues past age 5 or 6 is worth a closer look. This is especially true if your child has been dry before and then starts having accidents again. That pattern is called secondary enuresis, and it is often tied to something new happening in the body.
There are two types of bedwetting:
-
Primary enuresis: Your child has never consistently stayed dry at night.
-
Secondary enuresis: Your child was dry for at least six months but has started wetting the bed again.
Both types can be connected to how your child breathes at night.
What Is Sleep-Disordered Breathing in Children?
Sleep-disordered breathing (SDB) is a broad term for breathing problems that happen during sleep. This includes snoring, mouth breathing, and obstructive sleep apnea (OSA).
OSA happens when the airway becomes partially or fully blocked during sleep. The child's body struggles to get enough oxygen. This causes them to partially wake up, over and over, without fully remembering it.
Children are not small adults when it comes to sleep apnea. Their symptoms often look different. Instead of the classic daytime sleepiness you see in adults, children with OSA may show:
-
Snoring or noisy breathing at night
-
Sleeping with their mouth open
-
Restless sleep or unusual sleep positions
-
Bedwetting
-
Behavior problems or difficulty focusing during the day
-
Dark circles under the eyes
If your child has several of these signs, the connection between bedwetting and sleep apnea could be playing a role.
Why Does Breathing at Night Affect the Bladder?
This is the part that surprises most parents. When a child's breathing is disrupted during sleep, the brain shifts its focus to survival. Bladder control becomes less of a priority.
Here is what happens step by step:
-
The child's airway becomes partially blocked.
-
Oxygen levels in the blood drop.
-
The brain works harder to restore breathing.
-
Normal signals between the brain and bladder get interrupted.
-
The child does not feel the urge to wake up and urinate.
-
Bedwetting happens.
On top of that, when oxygen drops during these episodes, the body releases a hormone called atrial natriuretic peptide (ANP) . ANP increases urine production. So not only is your child unable to wake up to use the bathroom, but their body is producing more urine than it normally would overnight.
The combination makes nighttime dryness very hard to achieve.
How Common Is This Connection?
The research is detailed, and the numbers are hard to ignore.
A study published in The Journal of Pediatrics found that 41% of children referred to a sleep center for suspected sleep-disordered breathing were also actively wetting the bed. Children with a higher frequency of breathing disruptions per hour of sleep were significantly more likely to have bedwetting than those with normal breathing.
Research cited across multiple medical sources shows that up to 80% of children with bedwetting issues also have obstructive sleep apnea. That means for most children with persistent bedwetting, an airway problem is present at the same time.
These numbers suggest that bedwetting and sleep-disordered breathing are closely linked. Treating one without looking at the other means a lot of families never find a real solution.
Signs Your Child's Bedwetting May Be Related to Breathing
Use this table to see if your child's symptoms match the pattern seen in children with sleep-disordered breathing.
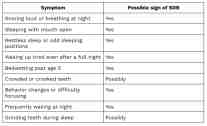
If your child shows three or more of these signs alongside bedwetting, it is worth talking to a dental or medical provider who understands airway health and can help identify the underlying reasons for bedwetting.
What Are the Common Bedwetting Solutions Parents Try First?
Most parents start with the basics. These include:
-
Limiting fluids after dinner
-
Waking the child up at a set time to use the bathroom
-
Using a bedwetting alarm that sounds when moisture is detected
-
Positive reinforcement and reward charts
-
Prescription medications to reduce nighttime urine production
These approaches can help in some cases. But they treat the symptom, not the cause.
If your child's bedwetting is linked to sleep-disordered breathing, none of these solutions will fix the root problem. You may see short-term improvement, but the bedwetting often returns.
What Does Airway-Focused Treatment Look Like?
When the airway is addressed, many children see a dramatic improvement in bedwetting. The goal of airway-focused treatment is to improve how your child breathes during sleep by addressing the physical structures of the mouth, jaw, and airway.
Depending on the child and the findings from an evaluation, treatment may include:
-
Oral appliance therapy: Custom devices worn during sleep that help keep the airway open and support proper jaw development.
-
Myofunctional therapy: Exercises that retrain the muscles of the tongue, lips, and face to support nasal breathing.
-
Referral to a physician: For children with confirmed OSA, collaboration with a sleep physician or ENT (ear, nose, and throat doctor) is part of a team approach.
-
Orthodontic evaluation: Crowded teeth or a narrow palate can contribute to airway restriction and may need to be addressed.
At Chester Dental Care , we work alongside other medical providers to make sure your child gets a full picture of their bedwetting treatment options, not just a dental perspective.
Why Does This Matter More Than Most Parents Realize?
Bedwetting is often dismissed as something kids grow out of. That is true for many children. But for children whose bedwetting is linked to sleep-disordered breathing, waiting it out means years of poor sleep.
Poor sleep affects more than just how tired your child is in the morning. Research consistently connects sleep-disordered breathing in children to:
-
Lower performance in school
-
Attention and behavior problems (often mistaken for ADHD)
-
Slower physical development
-
Weakened immune function
-
Emotional difficulties
Addressing the airway early can protect your child's health in ways that go far beyond dry sheets.
The good news is that children are still growing. Their jaw and airway structures are still developing. That means there is a window of time when support and treatment can make a lasting difference.
What to Do if You Think Breathing Is Behind Your Child's Bedwetting
If you have been asking " how do I stop bedwetting " and the common solutions are not working, start by looking at how your child breathes at night.
Watch them sleep for a few nights. Take notes. Listen for snoring. See if their mouth is open. Notice whether they seem to wake up easily or whether they stay very deeply asleep even when you try to rouse them.
Bring those observations to a provider who understands airway health. The more information you have, the better.
A dental provider with airway training can look at the structure of your child's mouth and jaw, screen for signs of sleep-disordered breathing, and refer you to the right specialist if a formal sleep evaluation is needed.
You do not have to figure this out alone.

Talk to an Airway-Focused Dentist in Chester, VA
Chester Dental Care works with families in Chester and nearby areas of Richmond, Chesterfield, Midlothian, and Hopewell, VA, who are looking for real answers to their child's sleep and health concerns.
With nearly two decades of dental experience, including close to a decade focused on airway and sleep dentistry, Dr. Shwetha Rodrigues takes a collaborative approach to care. We work alongside physicians, sleep specialists, and other providers to look at the whole picture.
If your child is wetting the bed and you want to understand whether breathing could be a factor, we are here to help.
Call us today at (804)748-2555 or email us at frontdesk@chesterdentalcareva.com to schedule an evaluation.
We serve families in Chester, Richmond, Chesterfield, Midlothian, Hopewell, and the surrounding areas of Virginia.