At Chester Dental Care , we work with families who have been told for years that bedwetting is “just a phase,” even when it keeps happening. Our focus on airway and sleep health has shown us that persistent bedwetting is often tied to medical causes that go beyond bladder development, including the link between bedwetting and sleep apnea. In this guide, we explain what we see in real patients, how breathing and sleep affect bedwetting, and why finding the root cause can make a lasting difference for a child’s health, confidence, and daily life.

Key Takeaways
-
Bedwetting that continues past age 7 may point to an underlying medical issue, not just slow development.
-
Sleep-disordered breathing is one of the most common medical reasons for bedwetting, affecting up to 80% of children with nocturnal enuresis.
-
A child who snores, mouth-breathes, or sleeps restlessly should be evaluated for airway problems, not just bladder issues.
-
Standard bedwetting solutions like alarms and fluid limits often fail because they don't address the root cause.
-
Treating airway and breathing issues can reduce or stop bedwetting without relying on long-term medication.
Is Bedwetting Normal, or Is Something Else Going On?
Bedwetting is common. In children under 7, it's usually a normal part of development. But when it continues past that age or returns after months of dry nights, it may be a sign of something medical.
About 5 to 7 million children in the United States deal with bedwetting at any given time. Around 20% of 5-year-olds still wet the bed, and up to 10% of 7-year-olds do as well.
Most parents are told to wait it out. And in many cases, that's reasonable. But some children have a medical reason behind their bedwetting that won't resolve on its own. Understanding the difference can save your child years of frustration, embarrassment, and lost sleep.
If your child wets the bed regularly and you're in the Chester or Richmond, VA area, this guide will help you understand what might really be going on.
What Are the Most Common Reasons for Bedwetting?
Bedwetting has several causes. The most common include deep sleep patterns, genetics, small bladder capacity, hormone imbalances, and sleep-disordered breathing.
Here's a breakdown of the main reasons for bedwetting in children:
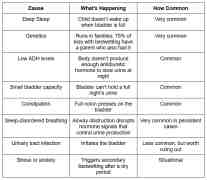
ADH (antidiuretic hormone) is a hormone your body releases to slow urine production during sleep. When a child doesn't make enough of it, or when sleep is disrupted, the body keeps producing urine at a normal daytime rate, even at night.
What Is the Connection Between Bedwetting and Sleep Apnea?
Children with sleep-disordered breathing, including obstructive sleep apnea (OSA), are at high risk for bedwetting. Research shows up to 80% of children with nocturnal enuresis have concurrent OSA.
Obstructive sleep apnea (OSA) is a condition where the airway becomes partially or fully blocked during sleep. This causes brief pauses in breathing, drops in oxygen, and fragmented sleep.
Here's why this matters for bedwetting:
When oxygen drops during an apnea episode, the body triggers a stress response. That stress causes the release of a hormone called atrial natriuretic peptide (ANP). ANP tells the kidneys to produce more urine. At the same time, the brain is so focused on drawing in oxygen that it stops monitoring other body functions, including bladder control.
The result? Your child's body is producing more urine than usual, while their brain is less likely to wake them up when their bladder is full.
Your child's bedwetting may not be a bladder problem at all. It may be a breathing problem; there is a clear correlation between bedwetting and sleep apnea .
Signs that sleep-disordered breathing could be behind your child's bedwetting include:
-
Snoring or mouth breathing during sleep
-
Restless sleep, tossing, and turning
-
Gasping or pausing during sleep
-
Waking up tired even after a full night's sleep
-
Difficulty focusing at school or behavioral issues
-
Crowded or misaligned teeth
How Do I Know If My Child's Bedwetting Is a Medical Issue?
If bedwetting continues past age 7, happens multiple times per week, or returns after a dry period, it's worth having your child evaluated for an underlying cause.
You don't have to catch your child snoring to suspect a breathing problem. Many kids with sleep-disordered breathing don't snore loudly. Instead, look for these patterns:
-
Bedwetting that doesn't respond to alarms, fluid limits, or rewards
-
Crowded teeth or a narrow jaw
-
Frequent mouth breathing during the day
-
Dark circles under the eyes
-
Behavioral issues that look like ADHD
A 2003 study published in The Journal of Pediatrics found that 41% of children referred to a sleep center for suspected sleep-disordered breathing were also wetting the bed.
That's not a small number. It means bedwetting and breathing problems are closely linked, and one is often hiding behind the other.
Why Do Standard Bedwetting Solutions Often Fall Short?
Bedwetting alarms, fluid restrictions, and medications treat the symptom. They don't address the underlying medical cause.
Standard bedwetting treatments include:
-
Moisture alarms – Wake the child when they begin to urinate. They work for habit-building but fail when the root cause is medical.
-
Fluid limits before bed – Reduce the volume of urine, but don't change how the bladder or brain responds to it.
-
Desmopressin (DDAVP) – A medication that mimics ADH to reduce nighttime urine. It helps control bedwetting but doesn't treat the cause.
These approaches can give families short-term relief. But if sleep-disordered breathing is behind the bedwetting, none of these tools fixes the problem. Children who fall into this category often keep wetting the bed, no matter how disciplined they are about routines.
This is the point where many parents feel stuck. You've tried everything. It keeps happening. That's the signal to look deeper.
What Does an Airway-Focused Dental Evaluation Have to Do With Bedwetting?
The structure of your child's jaw and airway directly affects how they breathe at night. A narrow jaw or crowded teeth can restrict the airway and contribute to sleep-disordered breathing.
Dentists trained in airway health look at more than teeth. They assess jaw development, tongue posture, nasal breathing patterns, and signs of sleep-disordered breathing. These are things that often go unnoticed in a standard pediatric checkup.
A narrow dental arch, for example, can limit the space available for the tongue and soft tissue in the airway. When a child sleeps, that tissue can collapse and obstruct breathing. Over time, this affects sleep quality, hormone regulation, and yes, bladder control.
At Chester Dental Care in Chester, VA, airway health is a core part of what we do. We work with parents to identify breathing issues that may be connected to bedwetting, sleep problems, and other symptoms that often get dismissed as behavioral or developmental.
Our team has nearly two decades of dental experience, with close to a decade focused on airway and sleep dentistry. We collaborate with other medical professionals to make sure your child gets care that addresses the whole picture, not just one piece of it.
What Are the Bedwetting Treatment Options Connected to Airway Health?
Bedwetting treatments that address the airway focus on improving nighttime breathing. This may include oral appliances, myofunctional therapy, or collaborative care with other providers.
Depending on what's found during an evaluation, airway-focused bedwetting solutions can include:
Oral appliance therapy: Custom-fitted dental devices can help support the jaw and airway during sleep, reducing obstruction and improving oxygen levels overnight.
Orofacial myofunctional therapy (OMT): OMT is a program of exercises that retrains the muscles of the tongue, lips, and face. It helps children breathe through their nose, close their mouth, and maintain proper tongue posture. All of these support a healthier airway.
Collaborative care: Because only a physician can diagnose and treat a sleep disorder, our team works directly with sleep specialists, pediatricians, and other professionals to make sure treatment is coordinated and appropriate for your child.
These approaches target what's happening in the airway, which in turn can help regulate the hormones and nervous system responses connected to bedwetting.
When Should You Stop Waiting and Talk to Someone?
Talk to a provider if your child is 7 or older and still wetting the bed more than once a week, if bedwetting has returned after a dry period, or if your child shows any signs of disrupted sleep.
Bedwetting is embarrassing. Kids feel it. Parents feel it too. The longer it goes on, the more it chips away at your child's confidence. Sleepovers get avoided. Self-esteem takes a hit. Bedwetting solutions are much needed.
You don’t have to wait for things to get worse or keep wondering, “ how do I stop bedwetting .” If your child is in Chester, Richmond, Chesterfield, Midlothian, or nearby areas in Virginia, Chester Dental Care offers airway-focused evaluations that look at the full picture of your child’s breathing, sleep, and dental health to help identify the real cause and guide effective treatment.

Talk to Chester Dental Care About Your Child's Bedwetting
Bedwetting that isn't responding to the usual approaches may be connected to how your child breathes at night.
At Chester Dental Care , we bring nearly two decades of dental experience and close to a decade in airway and sleep dentistry to every patient we see. We're Vivos clinical advisors, peer educators in airway dentistry, and active collaborators with other medical providers across the Richmond, VA area.
If your child snores, grinds their teeth, breathes through their mouth, or has teeth that aren't coming in right, those signs matter. So does the bedwetting.
Call us at (804)748-2555 to schedule an airway evaluation for your child. We are also available via email at frontdesk@chesterdentalcareva.com . We serve families in Chester, Richmond, Chesterfield, Midlothian, Hopewell, and nearby communities in Virginia.